Please note that some guidelines may be past their review date. The review process is currently paused. It is recommended that you also refer to more contemporaneous evidence.
Peripheral intravenous (IV) catheters are inserted into small peripheral veins to provide access to administer IV fluids (including dextrose and parenteral nutrition), medications, packed cell and blood product transfusions.
Blood required for diagnostic tests, including blood culture and venous blood gas can also be collected at the time of insertion.
IV cannulation definition of terms
Asepsis
Asepsis is the prevention of microbial contamination of living tissues or sterile materials by removal, exclusion or destruction of micro-organisms.
No-touch technique
The no-touch technique implies the use of sterile equipment, decontaminated hands and avoidance of surfaces or hands contacting exposed sterile equipment or sites. (This refers to the surfaces of sterile equipment that will come into contact with surfaces or sites that must remain uncontaminated to maintain asepsis).
These procedures require gloves if contact with blood or body fluids is likely.
Equipment for IV cannulation
The following equipment is required for IV cannulation:
- clean trolley
- sterile gloves (use standard precautions for all procedures where contact with blood possible)
- basic dressing pack
- 24 g Optiva or Insyte neonatal catheter
- blunt end drawing up needle
- 10 ml ampoule of 0.9% sodium chloride
- 2 x 2 mL syringes containing 0.9% sodium chloride, one to flush cannula and one to prime extension set
- 3-way stopcock (tap) if for continuous infusion
- skin antiseptic solution
- extension tubing
- tapes
- splint
- sterile occlusive dressing to cover the insertion point such as Tegaderm or IV3000.
Figure 1: Equipment for IV insertion
Technique for IV cannulation
Compared with adults, the veins in babies are smaller and poorly supported by surrounding soft tissue. A premature or sick infant may require multiple cannulations during a prolonged stay in intensive or special care and often veins that have previously been used, may need to be re-cannulated. Therefore, treat veins with respect!
Finding a suitable vein for cannulation
It is essential to spend time looking methodically for suitable veins. Points to note:
- Position the baby so you can see and have access to all limbs while ensuring that he/she is warm and well oxygenated (ideally a resuscitaire or incubator).
- Ensure good light: An angled procedure light is often better than the flat light built into the radiant heater.
- Take time and look at all the usual sites and choose the best option (see next section about preferred sites)
- Choose the vein carefully. A good vein
- runs straight
- stands up a little
- fills and empties
- is easy to splint
- In sick or smaller babies, try to avoid veins which are used to insert percutaneous central venous catheters. These include:
- the saphenous vein at the knee and ankle
- the cubital fossa
- the superficial temporal vein
- Repeat the process of looking if the attempt fails.
Figure 2: Visualising the vein
The preferred sites for IV cannulation
1. Hand
Dorsal arch veins
Dorsal arch veins are best seen on the back of the hand, but are usually larger and easier to see and palpate over the back of the wrist. Skin entry should be more distally. IVs inserted here are easily splinted and any infiltration easily spotted, so these veins are the preferred site.
The feeder veins over the dorsum of the hand in the first interspace need to be treated with respect, as it is possible to cannulate an artery here, risking loss of a thumb, or part thereof. (princeps pollicis artery). This is present in about 10% of infants. If present it is usually the sole supply to thumb.
Cephalic vein, in anatomical snuffbox
The cephalic vein is often quite large and can often be felt better than it can be seen. It is one of the veins to try if you must cannulate ‘blind’ in a large baby. Cannulas in this position tend to last quite well, making this a good secondary site. It can also be used for insertion of percutaneous central venous catheters.
2. Wrist
Volar aspect
Veins are easily seen on the volar side of the wrist. They are usually quite small and fragile and whilst easily cannulated, do not last well.
They are useful secondary sites, but must be carefully watched when noxious substances (eg Dopamine, Vancomycin) are infused, as they are prone to ‘burn’.
3. Cubital fossa
Median antecubital, cephalic and basilic veins
Median antecubital, cephalic and basilic veins are easy to hit and tend to last quite well if splinted properly. These veins are the preferred sites for insertion of percutaneous central venous catheters. These should be avoided unless absolutely necessary in any infant likely to need long term IV therapy.
The median nerve and brachial artery are both in the same anatomical vicinity and therefore vulnerable to damage.
4. Foot
Dorsal arch
Dorsal arch veins are small, but easily cannulated and last surprisingly well. The vein on the lateral aspect, running below malleolus, is easy to access, but must be splinted carefully and watched for infiltration.
Veins leading up to short saphenous are often good options.
Saphenous vein, ankle
The saphenous vein runs reliably just anterior to medial malleolus and is large and straight. It is easy to access and lasts well although is not always readily visualised. These veins are also good sites for insertion of percutaneous central venous catheters and should again be avoided in an infant likely to need long term IV access.
5.Leg
Saphenous vein at the knee
The saphenous vein runs just behind the medial aspect of the knee and is often visible behind the knee and as it curves around the top of the tibia. Access is easy and lasts well if properly splinted. However, this vein is a good site for the insertion of percutaneous central venous catheters and should be avoided if possible in any infant likely to need long term IV access.
6. Scalp
Scalp veins should only be used once other alternatives are exhausted. Mostly at least partial shaving of the head is required. It may take 6-12 months for hair to grow back properly, which may cause significant parental distress.
Superficial temporal vein
The superficial temporal vein runs anterior to the ear and is accessible over a distance of 5-8 cm in most babies and lasts well if secured appropriately This vein is also a good site for the insertion of percutaneous central venous catheters and should be avoided if possible in infants likely to need long term IV access.
The proximity of the temporal artery, which runs beside it, is a hazard. In small infants it can be almost impossible to tell the difference, even when the catheter has been inserted. It is important to try to identify the vessels separately, by careful palpation and by observation in a good light (in the smaller infants one can see the artery pulsate). If the catheter is in an artery, it must be removed.
Procedure
Ideally, the insertion of peripheral venous catheters should only be performed by a medical officer or registered nurse who has been accredited to do so.
Consider provision of pain relief consistent with the condition of the infant and the urgency of the procedure. Pain relief options are:
- application of 0.5 -1g EMLA to proposed site 60-90 minutes prior to insertion
- oral sucrose
- non-pharmacological settling techniques
Step-by-step procedure
Follow this procedure:
- Once through skin, stop and reorient the needle tip with regards to the vein. It is much easier if one advances directly over the vein, rather than from the side.
- Aim to enter the vein on a straight stretch.
- Advance in a stop-start fashion. Flashback is often rather slow, making it easy to inadvertently go straight through the vein.
- (In very small infants or with very bad veins you may not see blood return, but only be aware of a slight change in resistance as the needle enters the vein. If you wait a few seconds, blood sometimes appears, but do not rely on it. It may be necessary to try to advance the catheter without this confirmation.)
- Stop when blood appears. Check that needle is advancing along the line of the vein, correcting if necessary. Lift tip of needle slightly before advancing another 1-2mm. Check if bleeding into chamber continues, which confirms that the needle tip is still in the vein. Hold base of needle steady, push the canula off needle, either with the other hand or with the index finger of the same hand (the right if right-handed). Advance up the vein as far as it will easily go (preferably to the hub).
- If bleeding has stopped after initial small advance of the cannula/needle unit, it is likely that the needle tip is out of the other side of the vein. There is however a reasonable chance that the cannula tip is still within the vein. If the needle is pulled back into the cannula, blood might come up the cannula. If so, attempt to advance the cannula up the vein, leaving the needle in the cannula, but pulled back a little, to stiffen it.
- Release the tourniquet. Flush with 0.9% Normal Saline to check patency. If the cannula has not been fully advanced, flushing may also help to then advance it further up the vein.
- Remove any blood spills near insertion site before strapping.
- Without touching the insertion site use 2 Vee tapes around the end of the hub of the cannula.
10. Attach extension tubing and/or filter, and 3-way tap, securing Luer locks.
11. Splint: shape the splint to the limb and immobilise the joint above the insertion site (use smallest possible and avoid pressure areas). Tape loosely at the top and over the fingers. Place another notched tape a little more firmly over the hub of the catheter, so as not to obscure the insertion site itself. If necessary, place a piece of gauze between the hub and the skin so as to avoid a pressure area. Fingers/toes must be visible, as must the area around the catheter tip
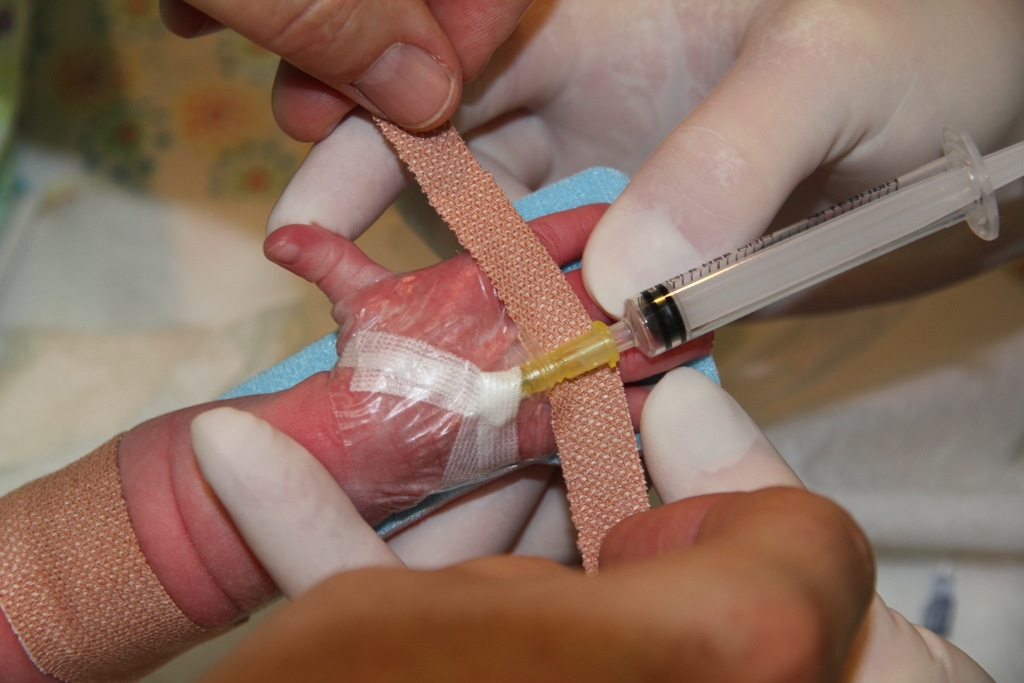 Figure 10: Attaching the splint 1
Figure 10: Attaching the splint 1
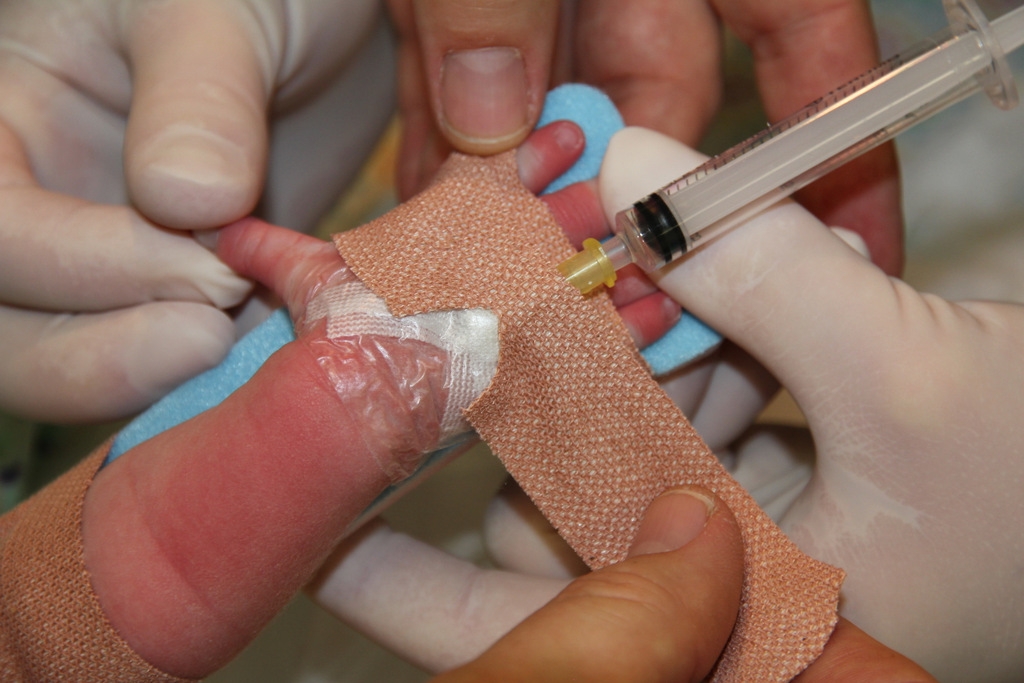 Figure 11: Attaching the splint 2
Figure 11: Attaching the splint 2
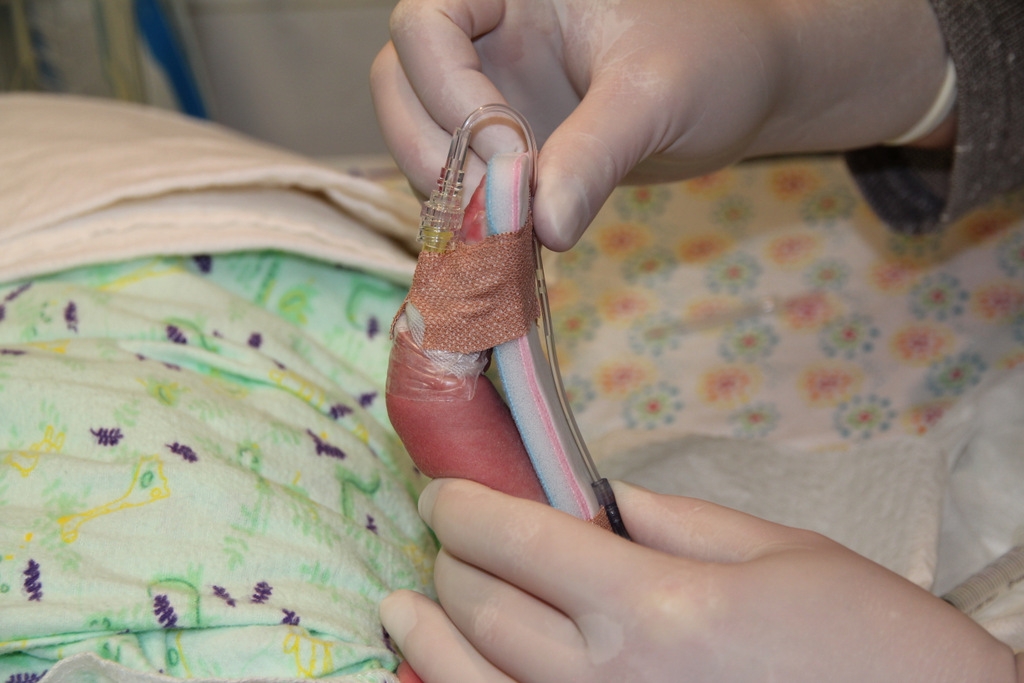 Figure 12: Attaching the splint 3
Figure 12: Attaching the splint 3
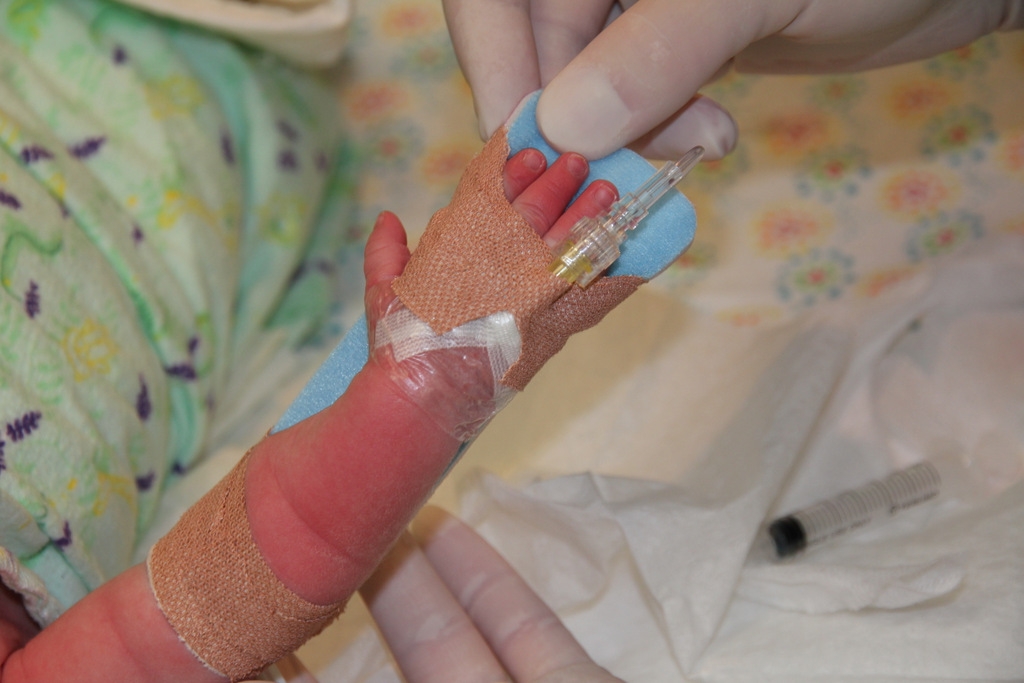 Figure 13: IV insertion complete
Figure 13: IV insertion complete
Start from step 1 for each attempt
For every additional attempt begin from step 1.
Avoid the temptation to use partly clean equipment as this increases the risk of infection.
N.B. A new cannula is required for each insertion attempt.
Potential complications of IV cannulation
Potential complications of IV cannulation include:
- phlebitis
- cellulitis
- sepsis
- tissue necrosis
- air embolus (incorrect priming).
The likelihood of phlebitis and sepsis secondary to IV cannulas can be reduced by electively resiting the cannula every 48-72 hours. This will depend to some extent on the availability of other sites.
If this approach is adopted, it is important to ensure that the new (replacement) IV cannula is in situ and functioning before the old one is removed (especially if the baby is nil orally and/or dependent on IV glucose to maintain glucose homeostasis).
More information
References
- Royal Women's Hospital (Melbourne, Victoria) Policy and Procedure Manual - Policy number 9W-04-2-049
- Mercy Hospital for Women (Melbourne, Victoria) Procedure Manual, 3rd Edition
- Royal Women's Hospital (Melbourne, Victoria) Parents information - IVs, drips and newborn babies
Thanks to Ballarat Health Services for providing all the images for this page.
Get in touch
Version history
First published: March 2014
Review by: March 2017

