Please note that some guidelines may be past their review date. The review process is currently paused. It is recommended that you also refer to more contemporaneous evidence.
All humans have diverse sex traits which are initially ambiguous in utero. For some humans, variations of natural ambiguity continue (whether related to chromosomal, hormonal or anatomical diversities). Ambiguous genitalia occur in approximately one in 4,500 births. This situation is rarely anticipated and it is important to reassure parents and staff that many ambiguous sex trait variations occur naturally in humans.
Issues relating to assigning sex
Often there can be perceived pressure on medical or nursing staff to 'make it better' and assign a sex to the child arbitrarily in the first few hours after birth. This is not helpful however and should be avoided. A careful clinical examination can be very informative. However to ensure the best decision is made for the child's gender, relevant tests often need to be completed, and the family and a multidisciplinary team of specialists should be involved in making a decision about the baby's sex or gender of rearing. Decisions will be informed by a combination of factors including external and internal genitalia, hormonal production and responses, reproductive potential and chromosomal make-up. It is important that parents are supported around this initial uncertainty as it is likely to be unexpected and can be a source of significant distress.
Choose your words carefully
It is important that clinicians and staff are mindful in their choice of words when discussing the baby with parents. It can be difficult not to discuss a baby without using gendered language such as 'he' or 'she', instead it is better to refer to the newborn as 'baby', 'child' or 'they'. Parents who are greatly distressed may assume that medical and nursing staff 'know' what the gender of the baby 'really is'.
Consequently any terminology used (deliberately or accidentally) may be given great emphasis by parents. This may lead to confusion and distress later if the suggested sex of rearing is at odds with initial 'off the cuff' remarks. If staff inadvertently use gendered language it is best to acknowledge that this was unintentional and that you do not have any insights that you are not sharing.
Advice on naming
Parents may seek advice regarding the naming of their infant. It is recommended that parents use an endearing name/nickname for the baby while waiting for the sex to be determined. This is common for many families who have not decided on a name for their baby.
Parents might not name the baby until the gender is known.
Management
Be very careful in your use of terms when discussing the baby with ambiguous genitalia.
Use the appropriate, non-gender orientated terms listed in Table 1.
Table 1: Suggested phenomenology when dealing with babies with ambiguous genitalia
| Female | Ambiguous | Male |
|---|---|---|
| She Clitoris Labia Ovaries Vagina, urethra | Your baby / they Phallus Folds Gonads Urogenital sinus | He Penis Scrotum Testes Urethra |
Never refer to the baby in question as ‘it’.
- Support and appropriate information sharing with parents around the reasons for variations in genital appearance is very important and should be undertaken early.
- It is important to consider that some babies with genital ambiguity may have associated medical conditions that need to be recognised early and treated appropriately to ensure the baby's wellbeing. The most commonly encountered such scenario is Congenital Adrenal Hyperplasia (CAH) in a baby girl, where in utero exposure to higher than usual levels of androgen result in ambiguity of the genital appearance.
- Early involvement of an experienced multidisciplinary team is important; advice from paediatric endocrinology should be sought early due to the risk of adrenal insufficiency in some scenarios, but also to help plan appropriate hormonal testing.
Clinical evaluation
Genital ambiguity can be quantified according to the Prader scale (see Figure 1).
Other relevant clinical details include:
- Are gonads palpable in the labioscrotal or inguinal regions? (Palpable gonads are likely to be testicular in origin; although these may not be fully developed.)
- Is penile length and width normal? (Length > 2.5 cm and < 4.5 cm in full-term infant; breadth usually ≥1cm.)
- Where is the urethral opening?
- Is there pigmentation of the genitalia?
- Are there syndromic features?
- What is the metabolic condition of the baby (paying particular attention to glucose, sodium and potassium)?
- Examine the baby's mother for signs of hyperandrogenism.
Care should be taken in the interpretation of examination findings in growth retarded or premature female neonates. These children often have very little labial fat, with a prominent clitoris, giving an appearance of ‘pseudo-ambiguity’. In addition biochemical parameters are different from preterm infants.
Breech delivery can result in clitoral and vulval oedema, again with the appearance of pseudo-ambiguity.
It is a moot point where the boundary lies between severe perineal hypospadias and genital ambiguity. Inability to palpate the gonads, a smaller than typical phallus or a bifid scrotum in this situation may be indicative of a diagnosis other than isolated hypospadias.
Figure 1: Prader staging system for the degree of virilisation of the external genitalia
Prader 0: Classical / typical female external genitalia
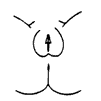
Prader 1: Female external genitalia with clitoromegaly
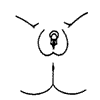
Prader 2: Clitoromegaly with partial labial fusion forming a funnel-shaped urogenital sinus
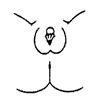
Prader 3: Increased phallic enlargement. Complete labioscrotal fusion forming a urogenital sinus with a single opening
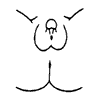
Prader 4: Complete scrotal fusion with urogenital opening at the base or on the shaft of the phallus.
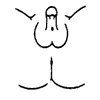
Prader 5: Classical / typical male external genitalia
Source: Prader Von, A. (1954). ‘Der genitalbefund beim Pseudohermaproditismus femininus des kongenitalen adrenogenitalen Syndroms. Morphologie, Hausfigkeit, Entwicklung und Vererbung der verschiedenen Genitalformen. Helv. Pediatr. Acta. 9: 231-248.)
Investigations
Appropriate investigations will vary depending on the clinical scenario. Advice on which tests will be helpful and the most appropriate timing for testing should be sought from a specialist team. Please note that hormonal testing should be deferred until at least Day 3 of life (and if low levels of gonadotrophins [± testicular hormones where Y material is present] are initially recorded then these should be repeated at ~2 weeks of life to confirm).
Investigations to consider include:
- chromosome analysis and FISH for Y (request urgent turn-around of FISH testing)
- blood glucose monitoring
- serum electrolytes (usually deferred until > 24hours unless otherwise indicated).
Hormonal testing - not all tests are needed in all scenarios.
For example testing of adrenal androgens is more important in babies without palpable gonads where CAH is being considered; in contrast for babies with a palpable gonad(s) but a smaller than typical penis / bifid scrotum, investigations concentrate more on the pituitary - gonadal axis.
Tests that may be considered in discussion with a paediatric endocrinologist:
- gonadotropins (LH, FSH)
- testosterone and dihydrotestosterone (after day 3; usually best to do with gonadotropins to optimise interpretation) ± oestradiol levels
- serum 17-hydroxyprogesterone (17OHP) ± androstenedione levels (after day 3 of life); these are not routinely needed if Y chromosome material is known to be present as CAH less likely
- Urinary steroid profile (after day 3 also).
Pelvic / abdominal / inguinal / groin ultrasound, carried out by an experienced sonographer, can be very helpful to determine:
- pelvic structures
- the presence or absence of gonads and their appearance and location.
Other investigations which may or may not be subsequently relevant include:
- sinugram
- human chorionic gonadotropin stimulation test (to assess testosterone and dihydrotestosterone synthesis capability)
- AntiMullerian hormone.
Differential diagnoses
Gonads palpable, 46XY:
- gonadal dysgenesis
- partial androgen insensitivity
- biosynthetic defect in either testosterone or dihydrotestosterone production
- pituitary hormone insufficiency.
Gonads impalpable, 46XX:
- congenital adrenal hyperplasia (CAH)
- gonadal dysgenesis
- exogenous androgen exposure.
Often only one gonad palpable, Mosaic karyotype:
- gonadal dysgenesis
- ovotesticular gonadal variation.
Ongoing management
Decision as to gender of rearing is made in conjunction with the family after opinions as to underlying reasons for the baby's genital variation have been sought from the endocrine and surgical teams.
The final decision rests with the baby's parents after all the relevant investigation results have been discussed.
Decisions as to sex of rearing will focus on the baby's best interests and highest likelihood of wellbeing.
The decision will be influenced by an amalgam of:
- the baby's karyotype
- gonadal status
- internal and external genital duct status
- potential for fertility and various future sexual functions
- cultural influences.
Birth certificate/registration
There is a 60-day period of grace between the birth of a child and when their birth certificate needs to be completed, so there is no rush. This can be deferred until a decision around gender of rearing has been made.
Long-term care
Issues to note:
- Families require long-term medical and psychological support.
- Infants, for example those with CAH have additional requirements for ongoing medical therapy.
- Disclosure to the patient about their diagnosis is usually undertaken in mid to late adolescence when they have the ability to understand complex issues such as chromosomes, hormones etc, and possess some degree of emotional maturity.
More information
Clinical
- UK guidance on the initial evaluation of an infant or an adolescent with a suspected disorder of sex development. Ahmed SF, Achermann JC, Arlt W et al. Clin Endocrinol (Oxf). 2011 Jul;75(1):12-26
- Changes over time in sex assignment for disorders of sex development. Kolesinska Z, Ahmed SF, Niedziela M, et al Pediatrics. 2014 Sep;134(3):e710-5
Consumer
- Parents information sheet
- Mayo clinic Ambiguous genitalia
- DSD Families website
- DSD Families - When your baby is born with genitals that look different... The first days
Additional resources
- AISSGA (Androgen Insensitivity Syndrome Support Group Australia) website
- OII (Organisation Intersex International Australi, info@oii.org.au
- Australian X & Y Spectrum Support (AXYS) website
- Genetic Support Network Victoria website
- Turner Syndrome Association of Australia website
- Better Health Channel for information about Androgen deficiency in men
- Orchids (documentary)
- XXY (movie, 2000)
- Intersection (movie 2012)
Parent fact sheet
Get in touch
Version history
First published: April 2015
Review by: February 2020

